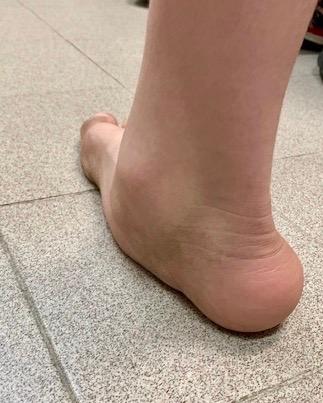
Flat feet are extremely common, in fact, toddler’s feet often look fat and flat. As we develop, in most instances, an arch develops. Flat feet or as they are often called excessively pronating feet can lead to a plethora of foot conditions and can ultimately lead to permanent deformities. In most cases, orthotics and insoles can help to control this excess motion; however, in some instances, orthotics cannot resolve the issue or orthotics cannot be tolerated.
What are some other names for flat feet?
You may hear flat feet described as pes planus, overpronation, excess pronation, hyper-pronation and fallen arches. They all ultimately describe the same condition.
What causes flat feet?
- In most cases, flat feet are simply the way that a person’s foot is designed to develop. It may be linked to genetics where the foot is designed to be positioned in this state by hereditary factors passed down by parents.
- Ligamentous laxity or as it is commonly called double-jointed occurs when the ligaments (little ropes that hold joints together) are too flexible or stretch too much.
- Following trauma. A motor vehicle accident or heavy fall may lead to tearing of the above-mentioned ligaments and fractures around the middle of the foot leading to sudden and very painful flat feet.
- Tarsal coalition.
- Arthritis that can lead to joint eventually collapsing.
- Being overweight can make a mildly flat foot worse.
What is Tarsal coalition?
This rare childhood condition often produces a rigid flat foot that is unresponsive to orthotics. As the foot is rigid, it cannot be corrected, and therefore orthotics tend to be painful and may not work. This condition occurs when two bones that should function separately begin to unite. This starts as a fibrous and flexible union and tends to progress over a 5-7 year process to be solid and fused. This foot is painful and impacts on all aspects of life.
There are two options for this condition – non-surgical treatment is to brace the foot and hold it in as straight a position as possible until the bones fuse. The foot would be fixed and rigid and depending on where the foot ends up can be mildly symptomatic or may impact on all aspects of walking and sport. However, if avoidance of surgery is important to the family, then this can be an option.
There is a surgical option in the form of resecting the coalition and mobilising the foot to free secondary contractures. Other procedures may be necessary at the time depending on the secondary deformities that may have developed while the foot was rigidly flat.
What is Posterior tibial tendon dysfunction
This can be a very severe problem leading to a complete collapse of the whole foot’s architecture. There are various stages of the condition, and it can ultimately lead to ADULT ACQUIRED FLAT FOOT.
This condition can be catastrophic if left to progress to the end stages. When identified early on, aggressive non-surgical treatment is imperative to try to prevent the end-stage. This may involve CAM boots, aggressive orthotics and physical therapy.
If the tendon damage progresses and the foot collapses, then surgery may be considered. The type of surgery carried out depends on how the foot has ended up. The aim of maintaining motion is paramount, and this can be achieved via a combination of procedures.
The tendon will be repaired, and then possible procedures involved may be HyProCure, medial calcaneal slide, Evans or Cotton procedures. If the foot has developed into the end stages, then fusion of the talonavicular joint may be required. This will be discussed later.
What are the signs of flat feet?
As flat feet are common, most people would recognise a flat foot. On weight-bearing, there should be an arch or upward curve present on the foot just behind the big toe joint and ending just in front of the heel. When the foot is flat, the arch collapses, and in severe situations, the inside of the foot sits on the ground. A bone may be prominent on the inside of the foot just below and in front of the ankle. This is typically only seen in marked flat feet.
Why do flat feet hurt?
Not all flat feet hurt, the world is full of people with flat feet who never even notice this. There is an ideal way for the body to function. Many years of research has lead us to understand how a foot should ideally work.
When the joints collapse and pass by their normal or ideal range of motion damage can start. The ligaments get constantly stretched, cartilage can be worn away, and muscles have to work too hard and overtime in an attempt to hold these joints together.
The study of biomechanics assesses the function and the forces that go through the body and how body parts interact. The way one section of the lower leg functions impacts on the way the other parts function; “The knee bone is connected to the foot bone” may be a childhood song; however, it is true.
When a foot flattens out, it leads to the knee rotating in too much and becoming excessively “knocked”. This abnormal motion can again damage the soft tissues that attempt to stop this, and the underlying joints can be damaged.
Why is it bad to have flat feet?
Having flat feet can lead to no pain; however, when the foot tends to roll in regularly, it can lead to the damage mentioned previously.
How do we diagnose flat feet?
Diagnosis is made by assessing how the foot functions by actively moving joints and in some situations measuring how these joints and body parts relate to each other.
The assessment will be done non-weight bearing plus an evaluation of the gait will be carried out. This means observing what happens to the feet and body when you walk or even run.
In some situations, weight-bearing X-rays may be necessary. This will allow us to see if there is an underlying problem with the bones and joints, such as tarsal coalition. It will enable us to measure the angles between bones to see how the foot various form the ideal situation.
What are the non-surgical treatments?
As flat feet are common, many devices have been developed over the years to help relieve pain or deformity.
- Typically, insoles or arch supports are simple devices that have an arch incorporated on them and simply try to hold the arch up.
- Orthotics/orthoses. These are are a more scientific way of supporting the arch. They can be custom made or semi-custom made. A podiatrist is the person to consult for these; they are university-trained professionals who will measure the foot angles and take a scan of the foot. This scan will be modified on a computer, and the orthotic will be prescribed and manufactured from this prescription. The technology for the manufacture has developed as all science and technology has and can now be digitally printed. Orthotics should be comfortable, fit in the shoes and control the foot.
- Quality shoes with a firm heel cup. These shoes, in conjunction with the foot orthotics, can help control the excess motion.
- Losing weight
- Specific exercises can help strengthen the foot; however, they cannot hold an arch up once it has collapsed.
Flat foot surgery and recovery
When to consider flat foot surgery?
If the above non-surgical attempts do not control the foot adequately, the symptoms cannot be controlled, or orthotics are uncomfortable, then there are surgical options. All attempts at non-surgical treatment are always strongly advised before surgery should be considered.
Can surgery fix flat feet?
Yes; various procedures have been developed today that can comfortably control the foot to allow for symptoms and deformity to be controlled.
What surgery is available?
Flexible flat foot
If the flat foot is completely reducible and flexible, i.e. you can raise the arch, then some of the minor minimally invasive procedures can be carried out.
HyProCure (arthroereisis)
In these situations, a minor procedure can be carried out. Utilising an incision approximately 10 mm a “stent” is inserted to painlessly control this motion, help resolve the issues and negate the need for orthotics.
A small “stent” is inserted between two bones, (not into a joint) to control how these bones are positioned in relation to each other. These stents are trialled in various sizes during the procedure until the correct control is established.
This can be carried out at the same time as other procedures or can be done as a separate stand-alone case. Patients can walk on the foot immediately in a firm dressing and post-op shoe, taking it easy for a few weeks until the small incision heals.
It must be mentioned that this procedure is not appropriate for all feet and during the initial assessment, a decision will be made as to the suitability.
See more here: http://www.hyprocure.com/flat-feet/
What is involved in the recovery after HyProCure flat foot surgery?
The surgery is carried out as a day surgery case, and there is no need for an overnight stay in the hospital. This surgery allows patients to be on their feet immediately following the procedure. In these instances, patients are expected to wear a post-operative protective shoe over their bandaging to protect the surgical site. In the first 3-7 days, patients are expected to rest as much as possible even though they can walk to the toilet or to perhaps make a cup of tea or heat a meal. At your first post-operative review (approximately seven days following the procedure), the dressing is changed, and at two weeks this large dressing is replaced by a minimal dressing following a daily saltwater soak. For most patients, a return to regular footwear occurs at about 3 to 4 weeks following the procedure, although this does vary from patient to patient.
When can I drive after the surgery?
It is typically advised to avoid driving while the large dressing is on and you are in the post-op shoe. This will mean you should avoid driving for about 2-3 weeks. This is often for safety reasons.
Is HyProCure surgery painful?
No. One of the main improvements in foot surgery is the marked reduction in pain. Pain is now controlled.
The incisions are very small, and a lot less damage is done during the operation.
The advancements in medication also allow pain not be an issue at all now. Some patients may require more intervention, however many patients experience no pain after the surgery.
Are other procedures required?
If the foot is not entirely flexible, then other minor procedures may need to be added to gain adequate correction. These are:
Cotton osteotomy
This is a relatively minor procedure involving making a cut into one of the bones on the arch and implanting a graft to reproduce an arch.
Evans osteotomy
Sometimes called a lateral column procedure. This is an excellent way of swinging the front of the foot back around to realign with the heel. A cut is made into the calcaneus or heel bone, and a graft is implanted to straighten the front of the foot.
What about in severe rigid flat feet?
In some instances where the foot has functioned markedly flat for many years, arthritis can develop and other conditions such as posterior tibial tendon dysfunction can develop, HyProCure is not appropriate. In these situations, more complicated procedures may be required, and often multiple procedures are necessary.
Talonavicular joint fusion
Once the tendon has lost function, and secondary damage to the other soft tissue restraining mechanisms develop, then it may be necessary to fuse this joint. This is a powerful procedure and allows the foot to be realigned and can avoid the triple arthrodesis that involves fusing three significant joints in the back of the foot. This will require more extended recuperation than the previously mentioned procedures, yet maybe a necessary life-changing procedure in certain situations.
Medial calcaneal slide
The heel bone is cut, and the back section is slid inwards to change the forces of the Achilles tendon and the other tendons around the foot.
Triple arthrodesis
This is the end stage surgery for a very painful, severely rigid deformed flat foot. Three major joints of the foot are fused. This is significant surgery with long recuperation; however, when the foot is severely impacting on the quality of life, this can be a life-changing procedure.
What complications can occur?
Modern foot surgery is very safe, and complications are now rare, although there are certain risks that patients must be made aware of, regardless of the rarity.
The risks of foot surgery are very similar to those risks posed by having other surgery, such as infection, unexpected pain, anaesthetic complications, contractures of the wound and unexpected scarring and deep vein thrombosis.
There are also risks associated with having certain medicines during and after your surgery, such as the possibility of nausea and vomiting.
There exist many very rare complications that can occur; these are very rare; however, they can occur.
Risks associated with surgery are explained to the patient during their pre-operative consultation. You will have every opportunity to ask as many questions as you like during the consultation.
Useful resources:
The Australasian College of Podiatric Surgeons
https://www.acps.edu.au/
The American College of Foot and Ankle Surgeons
HyProCure
